
PLEXIFORM NEUROFIBROMAS (PN) ARE PREVALENT AND PROGRESSIVE1
Prevalence


- PN are most likely congenital, and usually grow most rapidly during the first decade of life2
Progression
76% of patients with NF1 PN had tumor progression (defined as ≥20% volume increase per year) in a landmark, long-term Natural History study sponsored by the National Cancer Institute (NCI)*3,4
- Mean PN growth rate per year was 21.3%3
*The Natural History study began enrollment in 2008 and is ongoing. As of October 2018, 111 patients were enrolled who had NF-related PN. 92 patients with NF1-related PN between the ages of 3 and 18 years who had at least 2 volumetric scans during the Natural History study were included in the analyses above.3

Because PN grow rapidly in early
childhood,
timely evaluation and intervention are critical4

NATURAL HISTORY DATA SHOW THAT, IN GENERAL, PN GROW CONTINUOUSLY3
The Natural History study of patients with NF1-related PN began enrollment in 2008 and is ongoing. NCI volumetric MRI assessments up to October 15, 2018 were transferred to AstraZeneca, to allow analysis of PN growth of patients with NF1-related PN to serve as an external control for the SPRINT study. The following spider plot presents individual patient target PN volumes over 2.8 years3:
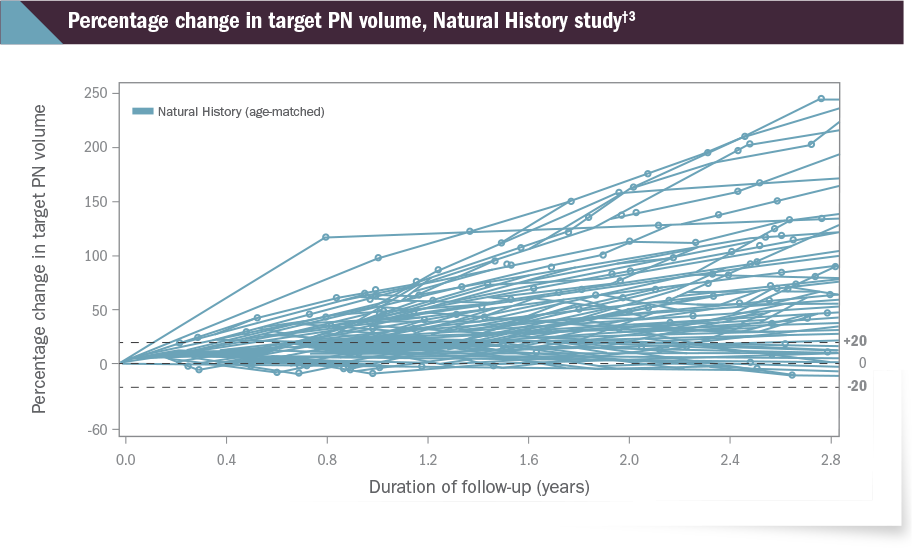
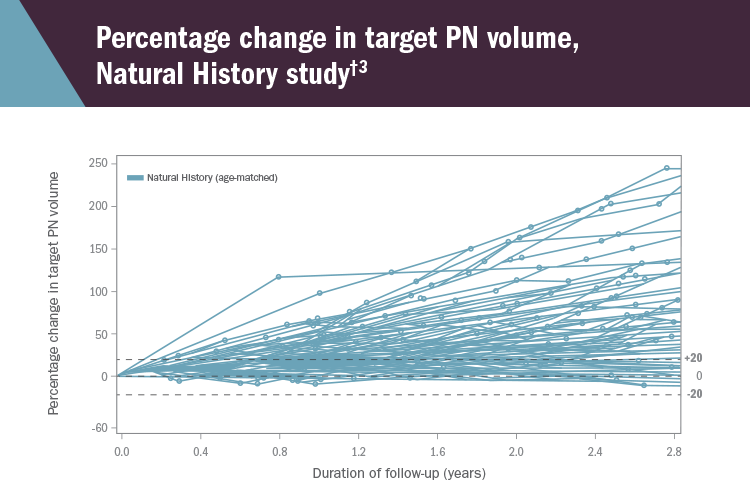
†92 patients are presented in this plot for the Natural History study. The full Natural History analysis set includes all patients with NF1-related PN (all ages) who have at least 2 volumetric MRI scans. The age-matched cohort includes a subset of the full Natural History analysis set including patients with at least 2 volumetric MRI scans where the first scan done within the age range of 3 to 18 years was considered the baseline.3
MRI=magnetic resonance imaging.
PN ARE A MAJOR SOURCE OF MORBIDITY
Clinical Complications


Motor dysfunction (functional impairment)1
- PN are invasive and can compress vital nerves and structures in the body, which can result in difficulty walking and loss of mobility

The presence of NF1 PN may result in tumor-related pain1,4,5
- PN-related pain has been shown to impair daily functioning
- Even small PN may cause pain depending on their location
- PN pain is commonly chronic. However, acute, sudden onset pain warrants an immediate tumor evaluation
- Some PN are undetectable by sight or touch and may only be noticed when they begin to cause pain

Disfigurement1
- PN tumors can result in visible deformities



PN-related morbidities may occur
or worsen as tumor volume
increases,
making early detection
and intervention critical4,5

THE SURGICAL DILEMMA OF PLEXIFORM NEUROFIBROMAS (PN)
Surgical Challenges

Post-surgical regrowth of PN is a common challenge6
- One retrospective analysis showed that 45% of PN regrew after surgery‡
Surgery can be challenging and PN may not be fully resectable due to1:
- Continuous growth within and throughout the nerve sheath
- Proximity to vital organs, which can occur initially or as the PN progress
- Poorly defined margins
- Challenging locations such as the head, neck, spine, or trunk
- Hypervascularity, which can increase the risk of bleeding during surgery

Surgery may not be an appropriate option for all patients6



‡Based on a retrospective review of the inpatient and outpatient records of 121 patients, who had 302 procedures on 168 tumors over a 20-year period at a single large pediatric referral center.6


